The value of mental health: where the burden sits and why it matters
Mental health rarely announces itself with a single dramatic moment. More often, its impact accumulates quietly – through days of reduced concentration, weeks of disrupted routines, and months of withdrawing from colleagues, friends, and daily life. Over time, this gradual detachment narrows opportunity: at work, at home, and in relationships.
In recent years, awareness has grown rapidly. Conversations that once felt difficult are now mainstream – in workplaces, schools, families, and boardrooms. But awareness alone isn’t enough. What matters most is whether that awareness translates into timely action – early enough to prevent short-term distress becoming lasting disengagement.
Why measurement matters
What we measure shapes what we prioritise. Much of the mental health debate still focuses on what is most visible: diagnoses, accessing treatment, and health care spending. But focusing narrowly on health budgets risks missing where the greatest losses occur – and where earlier intervention could preserve the most value.
That is why Zurich published The Value of Mental Health. While prevalence trends help establish scale, they only tell part of the story. Zurich's aim is not simply to count how many people are affected, but to quantify the everyday realities of mental health conditions for people, economies, and protection systems – including costs that fall outside formal systems, from wellbeing loss and workforce participation to informal care.
Zurich's report examines six countries – Australia, Chile, Germany, Malaysia, the UAE, and the UK. Despite very different national contexts, a consistent pattern emerges: the biggest costs sit upstream of healthcare spending.
Where the burden really sits
It starts with the individual – in the days when people struggle to function, concentrate, or manage everyday demands. On average, someone living with a mental health condition loses the equivalent of about two months of healthy life each year (measured in disability-adjusted life years). This is not time away from work or daily life, but reduced capacity and functioning spread across days, weeks, and months.
Scaled across populations, these losses far exceed spending on formal mental health care. They remind us that mental health is not just about illness or treatment, but daily functioning and quality of life.

Families and communities are often the first to absorb the burden, well before formal systems reach their limits.
Across all six countries, informal care from families and communities is one of the largest, least visible elements of support. In Malaysia, Chile, and the UAE, the estimated value of unpaid care provided by families exceeds public mental health spending.
When formal support is delayed or fragmented, families become the default safety net – absorbing care responsibilities that formal systems cannot meet at scale.
As the burden grows, it also impacts employers. Absence is visible and measured. But it accounts for only a small share of the total economic impact. The larger loss occurs when people struggle to stay connected to work – or never establish that connection at all.
In the UK, for example, just over half (53%) of people living with a mental health condition are in work, compared to 82% of those without one – a gap of 29 percentage points. While the gap is smaller in other countries, it remains significant.
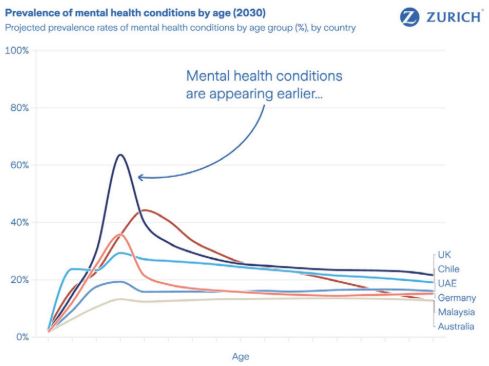
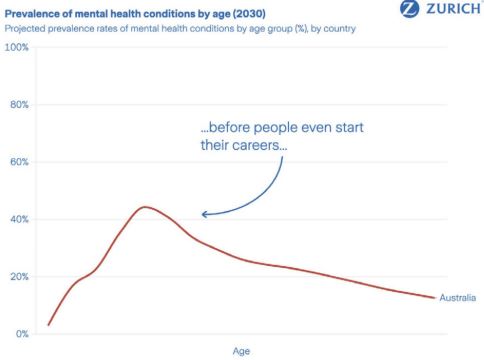
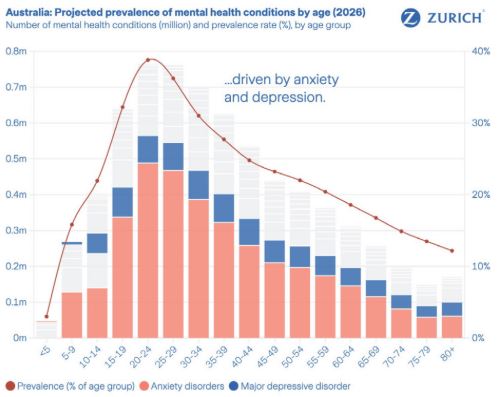
Most concerning, these patterns emerge earlier in life. In several markets, mental health conditions are now being identified before individuals enter the labour market, especially among adolescents and young adults. Early recognition can be a strength. But when support is delayed or poorly connected to education-to-work transitions, early distress can quickly become long-term disengagement.
What this reality means for employers
Employers aren’t being asked to “solve” mental health. But its consequences often become visible first in the workplace – where delays in support translate into lost participation and productivity.
Managers notice changes in performance and engagement. Teams absorb disruption. Organisations handle extended absences or challenging returns. All this tends to happen before someone reaches specialist care, and often after early warning signs.
That’s why timing matters.
As insurers – and as employers ourselves – we have a direct stake in understanding these pressures and how early action can improve outcomes.
Zurich's role isn’t to replace healthcare systems, but to help connect people to support earlier – reducing the risk that temporary distress becomes lasting disengagement. In practice, that includes workplace-linked support, early psychological intervention, and access to virtual care and counselling. When time away from work is needed, coordinated return-to-work pathways can make the difference between recovery and permanent exit.
Turning visibility into value
Awareness has brought the topic of mental health into the open. That’s real progress. But visibility alone doesn’t prevent loss. The next step is ensuring recognition translates into earlier action, stronger connection, and sustained participation – for people, for employers, and for society.
The Value of Mental Health asks: where is value being lost today – and where could it be better protected?
Because mental health shapes resilience every day. And when we act sooner and more effectively, we protect more of that value.
Supplied by REBA Associate Member, Zurich
At Zurich, we’re proud to have been providing UK insurance for over 100 years. Whatever you’re looking to support or protect, we’ll do our best to help you.






